A cure for baldness could be on the horizon thanks to a chemical used in McDonald’s fries.
Scientists have regrown hair in mice using a ‘simple’ technique – using human stem cells.
This generated fresh follicles capable of sprouting luxurious new locks. Within days the lab rodents had furry backs and scalps. Preliminary experiments suggest the groundbreaking therapy will also work in people. The Japanese team’s breakthrough came after they managed to mass produce ‘hair follicle germs’ (HFGs) in the lab for the first time. These are the cells that fuel follicle development. They are the ‘Holy Grail’ of hair loss research, as they have never been regenerated before.
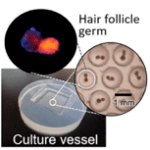
The secret was to use the ‘McDonald’s fries’ chemical dimethylpolysiloxane in the vessel in which they were cultured. This is added for safety reasons to prevent cooking oil from foaming. It was particularly effective for the HFGs because oxygen easily passes through.
Professor Junji Fukuda, of Yokohama National University, said: ‘The key for the mass production of HFGs was a choice of substrate materials for the culture vessel. ‘We used oxygen-permeable dimethylpolysiloxane (PDMS) at the bottom of culture vessel, and it worked very well.’ The method described in Biomaterials created up to 5,000 HFGs simultaneously – which led to new hair growth after they were transplanted into mice.

Billions of pounds are spent on hair loss treatments every year. Hair follicles have not been created this way before Prof Fukuda says hair loss troubles a substantial number of individuals all over the world, particularly in ageing societies.
Hair regenerative medicine has emerged as a new therapy to combat the problem. It involves regenerating hair follicles, the tiny organs that grow and sustain hair. But one of the more challenging obstacles has been the preparation of HFGs, their reproductive source, on a large scale. The researchers may have overcome this with a method that leads to a much more effective therapy. When they seeded the cells in a tiny ‘HFG’ chip called a 300-microwell array and injected them into mice it generated follicles and hairs on the body.
Prof Fukuda and colleagues reported black hairs on both the back and the scalp where they were transplanted. They said the ‘regenerated hair exhibited the typical hair cycle of mouse hair.’ Early tests have already indicated the technique will be just as successful on human skin cells. Prof Fukuda said: ‘This simple method is very robust and promising.
‘We hope this technique will improve human hair regenerative therapy to treat hair loss such as androgenic alopecia (male pattern baldness). ‘In fact, we have preliminary data that suggests human HFG formation using human keratinocytes and dermal papilla cells.’ He explained that his team mixed mouse skin cells with stem cells from mice and humans and seeded them in microwells in the custom-designed chip. Over three days the cells spatially separated from each other, exhibiting typical HFG features. Prof Fukuda said: ‘These self-sorted hair follicle germs (ssHFGs) were shown to be capable of efficient hair-follicle and shaft generation upon injection into the backs of nude mice.
‘This finding facilitated the large-scale preparation of approximately 5,000 ssHFGs in a microwell-array chip made of oxygen-permeable silicone. ‘We demonstrated that the integrity of the oxygen supply through the bottom of the silicone chip was crucial to enabling both ssHFG formation and subsequent hair shaft generation. ‘Finally, spatially aligned ssHFGs on the chip were encapsulated into a hydrogel and simultaneously transplanted into the back skin of nude mice to preserve their intervening spaces, resulting in spatially aligned hair follicle generation. ‘This simple ssHFG preparation approach is a promising strategy for improving current hair-regenerative medicine techniques.
This article was originally release by metro.co.uk
